Dental anxiety is far more common than many people realize. If visiting the dentist makes you tense or keeps you from getting care, the practice at Studio Dental Center for Advanced Dentistry offers proven ways to make appointments calmer and more effective. Our approach to sedation dentistry focuses on patient comfort, clear communication, and safe, evidence-based techniques that let you get the care you need with less stress.
Sedation is not a one-size-fits-all solution; it’s a tool we use selectively to remove barriers to treatment. Whether you need a single filling, a longer restorative appointment, or simply want a less anxious experience during routine care, sedation can reduce fear, limit memory of the procedure, and help patients tolerate treatment they’d otherwise avoid. Below, you’ll find clear, practical information about why sedation is used, how it works, and what to expect before, during, and after care.
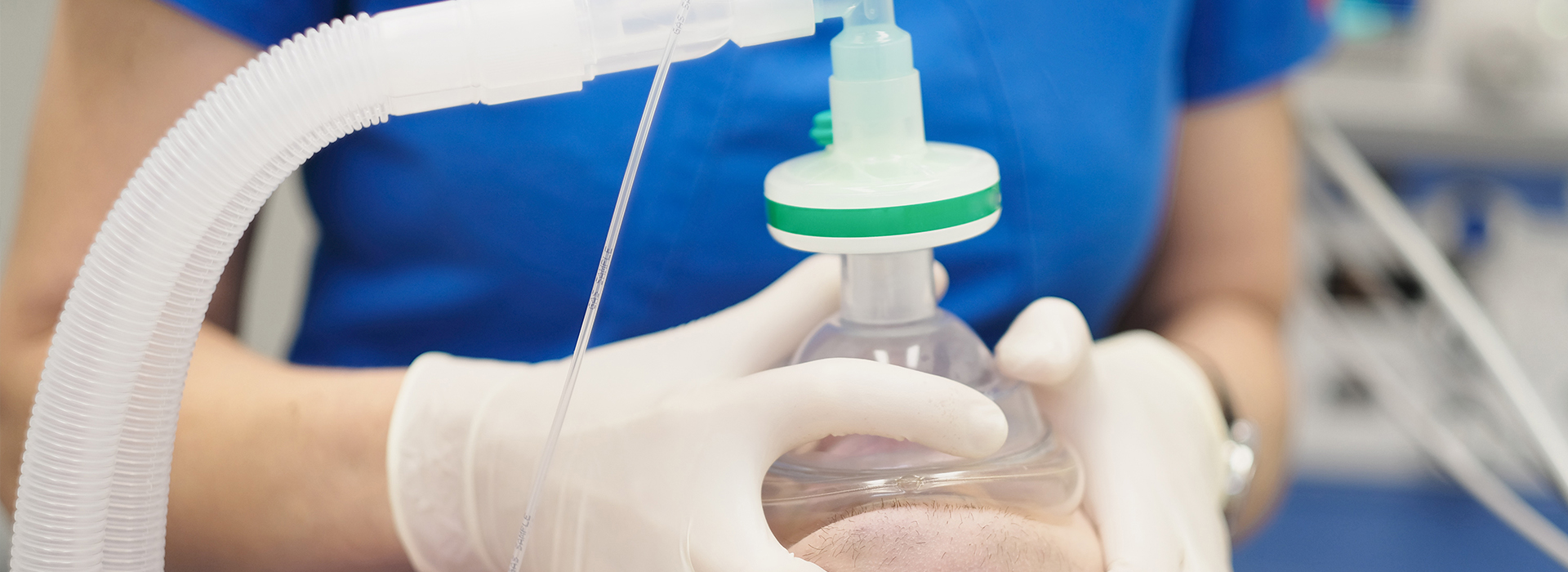
Sedation dentistry helps people stay relaxed during dental treatment by reducing the physical and emotional responses that make visits difficult. The goal is comfort — not unconsciousness for most patients — and to allow skilled clinicians to work more efficiently while you remain calm. Many patients describe the experience as pleasantly drowsy or simply detached from the details of the procedure, even when they are still responsive to instructions.
We always pair sedation with local anesthesia so you don’t feel pain in the treatment area. Sedation addresses the anxiety and sensory sensitivity that can make routine sounds and sensations feel overwhelming. By lowering fear and physical reactivity, sedation often improves cooperation and shortens the perceived duration of longer appointments.
Importantly, sedation is chosen with safety and appropriateness in mind. Your medical history, current medications, and specific dental needs guide the decision. Our team will review any health conditions and tailor the sedation plan so the experience is both comfortable and medically sound.
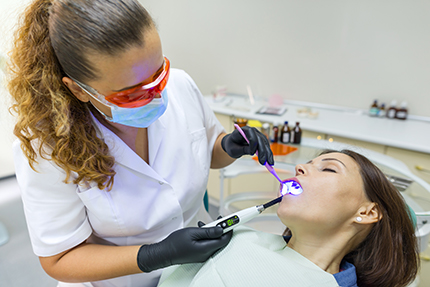
There are many reasons patients choose sedation beyond simple nervousness. For some, fear is so strong that routine exams and treatments are put off for years. For others, physical factors — a powerful gag reflex, sensitive teeth, or the need for extensive work in one session — make sitting through a procedure painful or impossible without help. Sedation offers a practical way to overcome these obstacles.
Severe dental fear — Sedation provides a pathway to care for people whose anxiety would otherwise cause them to avoid the dentist entirely, protecting oral and overall health.
Anxiety about a specific procedure — Even routine treatments can feel daunting. Sedation helps patients remain calm when they face extractions, root canals, or other procedures that trigger anxiety.
Long or complex appointments — When multiple steps must be completed in one visit, sedation can make the time more tolerable and reduce the need for multiple appointments.
Strong gag reflex or sensory sensitivity — For patients who struggle with gagging, hypersensitivity, or intolerance of dental instruments, sedation reduces reflexes and sensory distress so treatments can be completed comfortably.
Physical or cognitive limitations — Young children, people with certain disabilities, or patients with medical conditions that make holding still difficult can often receive needed care safely with appropriate sedation.
Everyone’s health and comfort needs are different, so we take an individualized approach when recommending sedation. A thorough medical and dental history, a review of current medications, and an assessment of past reactions to sedatives or anesthesia guide our recommendations. We’ll discuss the level of sedation appropriate for your treatment, explain potential risks, and answer any questions so you can make an informed decision.
Sedation choices balance effectiveness and safety. For many procedures, light or moderate sedation is enough to reduce anxiety without impacting vital functions. For patients who need deeper levels of sedation, we coordinate care to ensure continuous monitoring and the right clinical setting. Throughout, the aim is to match comfort with the safest possible plan for your situation.
Communication is a core part of personalization. Before any appointment that might include sedation, we’ll provide clear pre-visit instructions, review what to expect during recovery, and confirm any necessary arrangements like having a responsible adult accompany you home. That preparation removes surprises and helps create a smoother, more predictable experience.
It’s important to understand that much of dental sedation is "conscious," meaning patients maintain airway control and can respond to verbal cues while feeling relaxed or sleepy. Conscious sedation reduces anxiety and discomfort without the full loss of consciousness associated with general anesthesia. General anesthesia, which requires hospital-style monitoring and an anesthesia team, is reserved for cases where other methods are insufficient or when medical conditions dictate that approach.
Conscious methods are often safer for routine dental settings and allow patients to recover more quickly, while still providing the comfort needed for successful treatment. Choosing between conscious sedation and deeper anesthesia depends on the extent of the work, the patient’s health profile, and prior responses to sedative medications.
When conscious sedation is the right choice, we offer several methods tailored to the level of anxiety and the complexity of the procedure. These options can be adjusted by the dental team in real time, allowing for more or less sedation as needed. Below are the common approaches used in a modern dental practice.
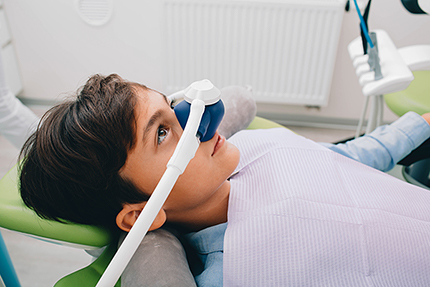
Nitrous oxide, commonly called "laughing gas," is inhaled through a small mask and provides mild relaxation that begins quickly and wears off almost immediately when the gas is stopped. It’s excellent for easing mild to moderate anxiety, reducing gag reflexes, and helping patients feel comfortable while remaining alert and cooperative.
Oral sedation involves a prescribed medication taken before the appointment to produce a calming, sometimes drowsy, state. The exact dose is chosen to match the level of anxiety and the expected procedure. Oral sedation usually requires a companion to drive the patient to and from the office and to remain available after the appointment.
IV (intravenous) sedation delivers medication directly into the bloodstream, allowing fast onset and precise control of the sedative level. IV sedation is used when deeper relaxation is necessary and can be adjusted during treatment to keep the patient comfortable. Because it produces stronger effects, specific pre-appointment instructions — such as fasting — and an escort home are required.
Your clinician will explain any special preparations for IV sedation, including timing for food and drink, medication adjustments, and post-procedure monitoring. These steps help ensure both safety and the best possible recovery.
Preparation is a shared responsibility between patient and care team. Before recommending sedation, we’ll review your medical history, any current prescriptions or over-the-counter medications, and recent health changes. This review identifies possible interactions and helps us select the safest sedation strategy. Honesty and clarity about your health history are essential for a safe outcome.
Some forms of sedation require specific instructions, such as avoiding food or drink for a certain number of hours before your appointment. Others may need a companion to drive you home and stay with you for a short time afterward. We’ll provide written and verbal instructions so you know exactly how to prepare and what to expect on the day of your visit.
Monitoring and emergency preparedness are part of routine sedative care. During sedation, we keep close watch on breathing, heart rate, and oxygen levels, and our staff are trained to respond quickly to any changes. These safeguards, combined with careful patient selection and clear pre-visit planning, make modern sedation dentistry both effective and safe.
Recovery from conscious sedation is typically quick, but patients may feel groggy for several hours. You should plan to rest for the remainder of the day and avoid driving, operating machinery, or making important decisions until you are fully alert. Follow-up instructions will cover pain control, activity limits, and signs to watch for that would warrant a callback.
We encourage patients to contact the office if they experience unexpected symptoms after sedation, such as prolonged dizziness, difficulty breathing, or severe nausea. Routine follow-up appointments allow us to assess how well the sedation and treatment met your needs and to make adjustments for future visits if necessary.
Our goal is to make dental care achievable, comfortable, and timely. If anxiety or physical challenges have kept you from getting the treatment you need, sedation can be an effective tool to bridge that gap. Contact us to learn more about sedation options and to discuss whether they might be appropriate for your next visit.

Sedation dentistry uses medications to reduce anxiety and increase comfort during dental procedures. Most approaches aim for relaxation rather than full unconsciousness, allowing patients to respond to verbal cues while feeling less aware of dental stimuli. Sedation is always combined with local anesthesia so the treatment area remains numb and pain-free.
By lowering fear and sensory reactivity, sedation often makes longer or more complex appointments tolerable and improves cooperation during treatment. The specific method and level of sedation are selected based on each patient’s health, treatment needs, and previous experiences with sedatives. Your clinician will explain the plan so you know what to expect before, during, and after care.
Conscious sedation produces a relaxed, drowsy state while patients retain airway control and can respond to verbal instructions. It reduces awareness of the procedure and may cause partial or complete amnesia for the appointment, but it does not typically render a patient fully unconscious. General anesthesia, by contrast, produces complete unconsciousness and requires hospital-style monitoring and an anesthesia team.
Because conscious sedation has fewer effects on vital functions, it is often safer and allows for faster recovery in an outpatient dental setting. The choice between conscious sedation and deeper anesthesia depends on the complexity of the procedure, the patient’s medical history, and prior responses to sedation. Your dental team will recommend the safest option for your situation.
Common conscious sedation methods include inhalation sedation with nitrous oxide, oral sedatives taken before an appointment, and intravenous (IV) sedation delivered during treatment. Nitrous oxide acts quickly and wears off almost immediately when stopped, making it useful for mild to moderate anxiety. Oral sedation provides calming effects for several hours and generally requires a companion to drive the patient to and from the office.
IV sedation offers fast onset and precise control of the sedative level, which can be adjusted in real time to match treatment needs. Each method has advantages and limitations, and the right choice depends on the expected procedure length, the degree of anxiety, and medical considerations. Your dental team will review these options and recommend a method that balances comfort and safety.
Candidates for sedation dentistry include patients with severe dental anxiety, those who have avoided care due to fear, and people who require long or complex procedures in a single visit. Sedation is also helpful for patients with a strong gag reflex, sensory sensitivities, or physical or cognitive limitations that make holding still difficult. The decision to sedate is individualized and based on a full medical and dental history.
Age alone is not always a limiting factor, but children and people with certain medical conditions may require specific considerations or coordination with medical providers. Your clinician will assess your overall health, medications, and prior responses to sedatives to determine whether sedation is appropriate and which level of sedation is safest. Clear communication about your health history is essential for a safe plan.
Personalizing sedation begins with a thorough review of medical history, current medications, allergies, and any previous reactions to anesthesia or sedatives. The dental team assesses the complexity and duration of the planned procedure, then recommends a sedation level that provides comfort while minimizing risk. Communication about expectations, pre-appointment instructions, and required post-appointment arrangements is part of the planning process.
At Studio Dental Center for Advanced Dentistry, we tailor sedation recommendations to match each patient’s needs and monitor responses closely throughout treatment. This individualized approach helps ensure the safest possible experience by balancing effectiveness with medical considerations. If deeper sedation is needed, the team coordinates additional monitoring and support as required.
Preparation varies by the type of sedation chosen but commonly includes fasting for a specified period before IV sedation and arranging for a responsible adult to drive you home after oral or IV sedation. You should bring a list of current medications and any recent changes to your health and follow any written pre-appointment instructions provided by the office. Honest disclosure of prescription, over-the-counter, and herbal supplements is important to avoid interactions.
Avoid alcohol and recreational drugs before sedation and follow guidance about taking routine medications the day of the appointment, which your clinician will review. Comfortable clothing and someone to escort you home contribute to a smooth experience. If you have concerns about preparation steps, contact the office in advance so staff can clarify instructions.
Modern sedation dentistry is safe when patient selection, dosing, monitoring, and emergency preparedness are handled by trained professionals. During sedation, clinicians monitor breathing, heart rate, blood pressure, and oxygen levels to ensure patient stability. Staff are trained to respond quickly to changes and follow established protocols for airway management and emergency care.
Choosing the right sedation level based on a complete medical history reduces risk, and written pre-visit instructions further promote safety. The office environment is equipped for monitoring and immediate intervention if necessary. If a patient’s medical profile suggests higher risk, deeper anesthesia may be arranged in a setting with advanced monitoring and an anesthesia team.
Recovery from conscious sedation is usually quick but can leave patients feeling groggy or mildly disoriented for several hours, depending on the medication used. Most people need to rest for the remainder of the day, avoid driving or operating machinery, and delay important decisions until they are fully alert. The dental team will provide written post-procedure instructions that cover activity limits, pain control, and signs that require a call to the office.
Some side effects, such as mild nausea or prolonged drowsiness, are possible and typically resolve within a day. If you experience prolonged dizziness, breathing difficulty, persistent vomiting, or other unexpected symptoms, contact the office promptly. Routine follow-up allows the team to evaluate how well the sedation met your needs and to plan adjustments for future visits if necessary.
Certain prescription medicines, over-the-counter drugs, and herbal supplements can interact with sedatives and change their effects, so a complete medication list is essential. Respiratory conditions, sleep apnea, uncontrolled cardiovascular disease, liver or kidney problems, and pregnancy are examples of health factors that influence sedation choices and may require special precautions. The dental team reviews these conditions to select the safest sedation approach and may consult with your physician when needed.
In some cases, adjustments to routine medications or additional monitoring will be recommended to reduce risk. Never stop or change prescribed medications without consulting the clinician who manages your care. Open communication about health history and ongoing medical treatment helps the team create an effective and safe sedation plan.
Yes, sedation can significantly reduce gag reflexes and sensory distress, making it easier to tolerate dental instruments and procedures. Nitrous oxide and other conscious sedation methods blunt reflex responses and lower anxiety, which often allows clinicians to complete necessary care that would otherwise be interrupted. For patients with heightened sensitivity, sedation can improve comfort and cooperation during examinations and treatments.
Specific strategies, such as combining topical anesthetics with conscious sedation, may further reduce discomfort during oral procedures. Your dental team will discuss which method is most appropriate based on the degree of sensitivity and the planned treatment. When needed, sedation can be an effective tool to ensure that patients receive timely, quality dental care without excessive distress.

Ready to book your next dental visit or have questions about your care?
At Studio Dental Center for Advanced Dentistry, our team is here to make getting started simple and stress-free. Whether you call, email, or submit our online form, we’re happy to help with scheduling, treatment questions, or anything you need along the way. We take the time to listen and guide you through your options so you feel confident and informed at every step. Take the first step toward a healthier, more confident smile, reach out today and experience personalized care made easy.