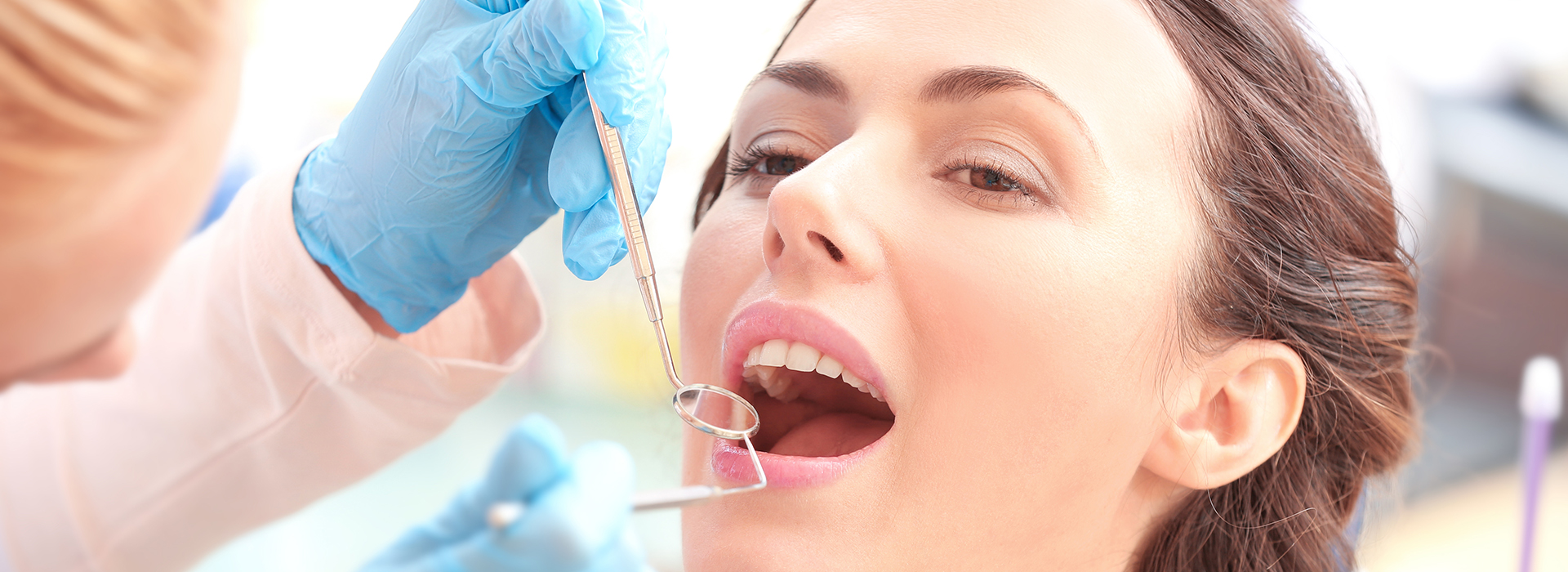
Gum disease is far more common than most people realize. Nearly half of adults over 30 in the United States show signs of periodontal disease, according to the Centers for Disease Control and Prevention. The condition ranges from mild, reversible inflammation to advanced infections that threaten the stability of teeth and the health of surrounding bone. At Studio Dental Center for Advanced Dentistry, we focus on clear explanations, careful diagnosis, and treatment plans designed to protect both your smile and your overall health.
Periodontal disease starts when bacteria in dental plaque build up along the gumline. These bacteria provoke an inflammatory response in the soft tissues around the teeth. Left unchecked, this inflammation can cause the gum tissue to separate from the tooth, forming pockets where bacteria multiply and deeper infection follows.
The early stages are often subtle: you might see a little redness or notice gums that bleed occasionally. Because symptoms can be mild or intermittent, many people don’t realize a problem exists until it has progressed. That’s why consistent home care combined with professional monitoring is crucial.
Controlling plaque, interrupting the bacteria-host response, and maintaining tissue health are the essential steps in stopping disease progression. Early intervention makes a dramatic difference in outcomes; in many cases, simple, conservative treatment can return the gums to a healthy state.
Indicators of gum disease may include:
Red, swollen, or tender gums
Bleeding during brushing or flossing
Gum recession or exposed tooth roots
Increased tooth sensitivity to hot and cold
Persistent bad breath or a bad taste in the mouth
Loose teeth or changes in how teeth fit together
Pus or discharge around the teeth and gums
New spaces forming between teeth or changes in partial denture fit

Healthy gums do more than hold teeth in place — they help protect the body from chronic inflammation and bacterial spread. Research continues to reveal connections between periodontal inflammation and systemic conditions such as cardiovascular disease, diabetes complications, and respiratory issues. Managing gum health is therefore an important part of preserving general well-being.
When gum tissue becomes chronically inflamed, the immune response can create a persistent state of stress on the body. Reducing that inflammation through effective periodontal care can improve not only oral comfort and function but also broader markers of health in many patients.
Our approach emphasizes prevention and early detection, with personalized guidance on daily care and regular professional evaluations. By partnering with patients, we aim to preserve natural teeth, limit the need for more invasive treatment, and support long-term health.
Gingivitis is the first, reversible stage of gum disease. It is characterized primarily by inflammation without irreversible loss of bone or connective tissue. Common signs include gum redness, puffiness, and bleeding with brushing; some people also notice bad breath that doesn’t respond to rinses alone.
The good news is that gingivitis responds well to consistent improvements in oral hygiene and professional cleanings. A focused routine of twice-daily brushing with attention to the gumline, daily interdental cleaning, and regular dental checkups usually resolves the inflammation and restores healthy tissue.
Identifying gingivitis early gives you a better chance of avoiding the more destructive phases of periodontal disease. We emphasize education and practical coaching so patients can make small changes that have long-term benefits.

When gingivitis is not controlled, it can progress to periodontitis, a condition in which the supporting structures of the teeth — the ligaments and bone — are damaged. This stage involves deeper pockets between the tooth and gum, gradual bone loss, and an increased risk of tooth mobility and eventual tooth loss if left untreated.
Periodontitis is not a single, uniform disease; it varies in severity and pattern from patient to patient. Treatment goals focus on stopping the active infection, reducing pocket depth to enable effective cleaning, and, when necessary, attempting to regenerate lost tissues to restore support.
Early diagnosis and a tailored care plan are critical. With timely intervention, many patients preserve their natural dentition and avoid the complications that follow untreated disease.
Treatment for gum disease is pragmatic and staged. We begin with the least invasive, evidence-based options and escalate only when necessary. The plan for each patient depends on the severity of disease, the anatomy of the mouth, systemic health factors, and individual treatment goals.
Open communication is central to our process: you’ll understand why each recommended step matters, what results to expect, and how to maintain improvements once treatment is complete. Collaboration between patient and clinician is the most reliable path to lasting periodontal health.
Below are the general pathways we follow to restore and maintain healthy gum tissue.
In many cases, non-surgical management is the first and most effective option. This includes thorough, targeted cleanings known as scaling and root planing, which remove plaque and hardened deposits from below the gumline and smooth root surfaces to discourage bacterial recolonization.
Adjunctive measures may include local antimicrobial agents placed in pockets and personalized hygiene coaching to improve daily plaque control. These steps can reduce pocket depth, decrease inflammation, and often restore healthy attachment when started promptly.
Regular periodontal maintenance after initial therapy is essential; ongoing cleanings and monitoring help sustain gains and detect any recurring activity early.
When pockets are too deep to be cleaned effectively with non-surgical methods (commonly when pocket depth exceeds practical reach), surgical intervention may be recommended. Procedures such as flap/pocket reduction surgery allow direct access to remove bacteria and recontour infected tissues to reduce pocket depth and improve cleaning ability.
Contemporary periodontal care also employs regenerative techniques — bone grafts, barrier membranes, and biologic agents — to encourage the restoration of lost bone and connective tissue when conditions are favorable. These therapies aim to rebuild support and improve long-term prognosis for affected teeth.
In select cases, laser-assisted procedures can complement traditional surgery by reducing bacteria and promoting tissue healing. Our treatment plans are individualized, and we’ll explain the rationale and potential benefits of each option.
Successful periodontal care doesn’t end with a single procedure. Long-term health depends on consistent home care, regular professional maintenance visits, and attention to medical factors that influence periodontal stability. Smoking cessation, diabetes control, and other lifestyle changes can play a major role in preventing recurrence.
At Studio Dental Center for Advanced Dentistry, we work with patients to build realistic, sustainable routines and a maintenance schedule that matches their individual risk. Early detection during routine appointments allows us to intervene promptly and preserve the outcomes of treatment.
If you have concerns about bleeding gums, loose teeth, persistent bad breath, or any other signs described on this page, please contact us to learn more about how periodontal care can protect your smile and support your overall health.

Periodontal disease describes a range of inflammatory conditions that affect the gums and the supporting structures of the teeth. Gingivitis is the earliest, reversible stage and involves inflammation of the gum tissue without loss of bone or connective tissue. When gingivitis is not controlled it can progress to periodontitis, which involves deeper infection, pocketing, and potential bone loss.
Early identification of gingivitis often allows resolution with improved home care and professional cleanings, while periodontitis typically requires more intensive therapy to control infection and preserve support. The distinction guides treatment choices and expected outcomes. Understanding these stages helps patients and clinicians select timely, appropriate care to protect natural teeth.
Gum disease begins when bacterial plaque accumulates along the gumline and provokes an immune response in the soft tissues. That inflammatory response can damage the attachment between tooth and gum, creating pockets where bacteria multiply and escape routine cleaning. Risk factors such as tobacco use, uncontrolled diabetes, certain medications, and genetic predisposition can increase susceptibility and accelerate progression.
As pockets deepen, they shelter bacteria and make mechanical cleaning less effective, which perpetuates inflammation and tissue breakdown. Interrupting this cycle through plaque control and professional therapy is essential to stopping disease progression. Regular monitoring allows clinicians to identify areas of active disease and adjust care accordingly.
Common early signs include red, swollen, or tender gums and bleeding during brushing or flossing. Patients may also notice persistent bad breath, increased tooth sensitivity, gum recession exposing root surfaces, or changes in how teeth fit together. Because symptoms can be mild or intermittent, many people do not recognize a problem until disease has advanced.
If you observe these signs, prompt evaluation helps determine whether gingivitis or a more advanced form of disease is present. A clinical exam and, when appropriate, radiographs provide information about inflammation and bone health. Early intervention generally improves the prognosis for maintaining natural dentition.
Diagnosis begins with a comprehensive periodontal exam that includes probing pocket depths, measuring attachment levels, and assessing gum inflammation. Digital radiographs or CBCT imaging may be used to evaluate bone levels and detect areas of bone loss not visible on a visual exam. Your clinician will also review medical history, medications, and risk factors that influence disease activity and healing.
This combination of clinical measurements, imaging, and history allows the team to stage disease severity and develop an individualized treatment plan. Ongoing assessment over time identifies recurrent inflammation and guides maintenance intervals. Clear communication helps patients understand findings and participate in decision-making.
Non-surgical therapy is often the first line of treatment and includes scaling and root planing to remove plaque and hardened deposits from below the gumline. Smoothing the root surfaces helps discourage bacterial recolonization and allows tissue to reattach where possible. Adjunctive measures such as local antimicrobial agents or antiseptic rinses may be used to reduce bacterial load in targeted areas.
Personalized hygiene coaching is a key component of non-surgical care and helps patients improve daily plaque control. After initial therapy, periodontal maintenance visits are scheduled to monitor healing and prevent recurrence. Many patients achieve stable gum health with diligent home care and regular professional follow-up.
Surgical intervention is considered when pocket depths or anatomic factors prevent thorough cleaning with non-surgical methods. Procedures such as flap surgery reduce pocket depth and recontour infected tissues, while regenerative techniques like bone grafting and barrier membranes aim to restore lost bone and connective tissue when conditions are favorable. In selected cases, laser-assisted procedures can complement traditional surgery by reducing bacteria and promoting tissue healing.
The primary goals of surgical care are to eliminate persistent infection, create a healthier architecture for cleaning, and, whenever possible, rebuild support to improve long-term prognosis. Success depends on careful case selection, patient health, and adherence to maintenance. Your clinician will explain the expected benefits, limitations, and required follow-up for any recommended procedure.
Chronic periodontal inflammation contributes to a systemic inflammatory burden and has been associated with conditions such as cardiovascular disease, complications of diabetes, and certain respiratory issues. While these relationships are complex and not uniformly causal in every individual, reducing oral inflammation can lower systemic markers of inflammation for many patients. Recognizing the oral-systemic link helps prioritize periodontal care as part of whole-health management.
Patients with systemic conditions often require tailored periodontal plans that consider medications, healing capacity, and overall risk. Effective periodontal management can be an important component of broader medical care, and coordination between dental and medical providers enhances patient outcomes. Addressing modifiable risk factors such as smoking and poor glycemic control further supports both oral and systemic health.
Periodontal maintenance is a program of regular professional cleanings and monitoring scheduled according to individual risk and disease history. Visits commonly occur every three months during the initial stabilization phase and may be extended if clinical stability is achieved, but intervals are always personalized based on ongoing findings. Maintenance appointments include targeted cleaning, reassessment of pocket depths, and reinforcement of home care techniques.
Consistent adherence to recommended recall intervals is the most reliable way to preserve treatment gains and detect recurrent activity early. During maintenance the team can treat minor flare-ups promptly and adjust the care plan as needed. Long-term success depends on the partnership between patient and clinician to sustain healthy tissues.
Effective prevention centers on consistent daily plaque control: twice-daily brushing with attention to the gumline, daily interdental cleaning, and use of appropriate oral hygiene aids for your anatomy. Choosing the right interdental tool—floss, interdental brushes, or a water flosser—should be guided by your clinician to ensure thorough cleaning between teeth. Lifestyle choices such as avoiding tobacco, maintaining balanced nutrition, and controlling systemic conditions like diabetes also support healthier gums.
Regular professional cleanings remove deposits that are difficult to eliminate at home and allow early detection of changes that signal disease activity. Patient education and periodic reinforcement from the dental team help translate good habits into lasting results. Preventive-focused care is the most effective way to avoid invasive treatments and preserve natural teeth long term.
Adults who notice bleeding gums, persistent bad breath, gum recession, loose teeth, or who have risk factors such as smoking or diabetes should seek a periodontal evaluation. Even patients with subtle symptoms benefit from assessment because early intervention improves outcomes. A thorough exam will determine whether conservative or more advanced therapy is indicated based on clinical findings and medical history.
For a periodontal consultation bring a list of current medications and relevant medical history, and be prepared to discuss symptoms and oral hygiene habits. At Studio Dental Center for Advanced Dentistry in Plantation, FL, the team will perform a focused exam, explain findings, and outline a personalized plan tailored to your needs. If additional imaging or specialist care is recommended, the office will coordinate the next steps and clarify follow-up expectations.

Ready to book your next dental visit or have questions about your care?
At Studio Dental Center for Advanced Dentistry, our team is here to make getting started simple and stress-free. Whether you call, email, or submit our online form, we’re happy to help with scheduling, treatment questions, or anything you need along the way. We take the time to listen and guide you through your options so you feel confident and informed at every step. Take the first step toward a healthier, more confident smile, reach out today and experience personalized care made easy.