
At the office of Studio Dental Center for Advanced Dentistry, patient comfort and long-term oral health guide every recommendation we make. Although our primary goal is to preserve natural teeth whenever possible, there are times when extraction is the most responsible, predictable way to protect a person’s smile and overall wellbeing. When removal is advised, we focus on clear communication, gentle technique, and thoughtful planning so patients know exactly what to expect.
Deciding on an extraction is never taken lightly. Our team evaluates your oral condition in the context of your medical history, existing dental work, and future restorative goals. That comprehensive approach helps us determine whether a tooth can be repaired or whether removing it will prevent further problems such as infection, shifting of adjacent teeth, or ongoing discomfort.
We also prioritize comfort and safety. Before any procedure, we review options for anesthesia and sedation, explain the steps of treatment, and outline the recovery process. Our emphasis on preparation and patient education helps reduce anxiety and supports a smoother, more predictable healing period.
Persistent baby teeth that block permanent eruption
Sometimes a primary tooth fails to loosen or its roots do not resorb as they should. An over-retained baby tooth can interfere with the normal eruption path of its permanent replacement and may lead to misalignment or space problems. When monitoring shows that removal will benefit dental development, extracting the baby tooth is the most direct solution.
Permanent teeth that are extensively decayed and cannot be restored
Decay can progress from a small enamel defect to severe structural loss when left untreated. When a tooth has lost too much healthy structure or the nerve and supporting anatomy are compromised beyond repair, extraction is often the safest option to stop infection and protect surrounding teeth and tissues.
Teeth that are fractured or cracked beyond practical repair
Teeth can sustain a variety of fractures. When the damage extends into the root or when the remaining structure cannot reliably support a crown or other restoration, extraction prevents repeated procedures and ongoing pain or infection.
Advanced periodontal disease with loss of support
Severe gum disease erodes the tissues and bone that hold teeth in place. In advanced cases, teeth become mobile and painful; removing teeth that no longer have adequate support can halt disease progression and make future restorative or periodontal work more effective.
Wisdom teeth that are impacted, decayed, or causing harm
Third molars often lack the room to erupt normally and can press on neighboring teeth, trap debris, or develop infections. In many situations early removal prevents future complications and preserves the health of adjacent teeth.
Extractions performed as part of orthodontic planning
When the jaws do not provide enough space for all permanent teeth, selective removal can create the room needed to align teeth properly and establish a balanced bite as part of an orthodontic treatment plan.
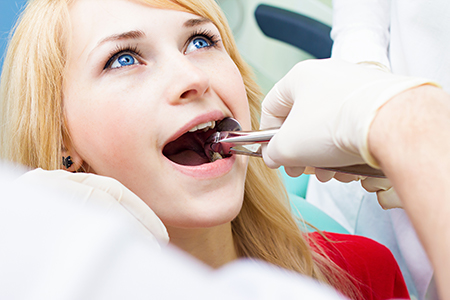
Careful planning is the foundation of a successful extraction. Our dentists begin with a focused clinical exam and a review of your medical history, including current medications and any systemic conditions that could affect healing. That information helps us decide whether additional precautions, referrals, or medical clearance are necessary before proceeding.
Imaging plays an important role in planning. We use digital radiographs—and when needed, three-dimensional CBCT scans—to visualize root shape, the proximity of nerves or sinuses, and the quantity of surrounding bone. This level of detail helps us choose the safest, least invasive approach for each case.
We also discuss anesthesia and comfort options tailored to your needs. Local anesthetic is standard, and for patients with dental anxiety or for more complex cases, we can offer dental sedation to make the experience more comfortable. If a case requires specialist care, we coordinate referrals so you receive the appropriate level of surgical support.
Extractions fall into two broad categories: straightforward removals and surgical extractions. For either type, our priority is to control discomfort and protect surrounding structures. We begin by ensuring the area is completely numb and confirming that you are comfortable with the planned approach and any sedative options.
During the procedure, the dentist will use gentle, controlled motions to separate the tooth from its ligaments and supporting bone. When a tooth is fully erupted and has uncomplicated root anatomy, forceps are usually sufficient to remove it efficiently and with minimal trauma.
For patients who need extra support, we will explain the reasons for a referral to an oral surgeon. Referrals are made when a tooth’s position, root configuration, or involvement with adjacent anatomy would be best managed by a specialist. Our team will coordinate care and share all necessary records to ensure continuity and a positive outcome.
A simple extraction applies when the tooth is visible in the mouth and the roots are straightforward. After administering a local anesthetic, we loosen the periodontal fibers and remove the tooth using appropriate instruments. Throughout the procedure we monitor your comfort and adjust anesthesia or add sedation as needed to keep you relaxed.
Simple extractions typically require minimal intervention and allow for a quick recovery. We will review post-extraction instructions with you and schedule any needed follow-up to confirm healing and discuss whether and when to replace the missing tooth.
Surgical extractions are indicated for teeth that are broken at the gumline, ankylosed (fused to bone), or impacted. These procedures often require a small incision in the soft tissue and, in some cases, precise removal of a small amount of bone to access the tooth. Local anesthetic is used to prevent pain, and sedation can be arranged if appropriate.
When a complex extraction is involved, we may work with an oral and maxillofacial surgeon to ensure the safest technique and best possible outcome. Surgical removal is performed with careful attention to preserving surrounding tissues and planning for predictable healing and future restoration.
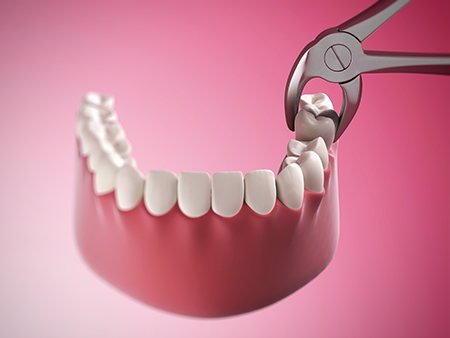
Recovery times vary by the type of extraction and the individual patient, but most people can expect the first two to three days to involve the most noticeable discomfort and swelling. We provide clear post-op instructions to control bleeding, minimize swelling, and reduce the risk of complications. Following those directions closely supports faster, more comfortable healing.
It’s important to monitor the extraction site and follow medication instructions when prescribed. If stitches were placed, we will explain whether they will dissolve on their own or require removal at a follow-up visit. Keeping the area clean without disturbing the healing clot is a key part of preventing complications like dry socket.
If you have unusual symptoms such as persistent heavy bleeding, increasing pain, or signs of infection, contact our office promptly so we can assess the situation and provide timely care. Most post-operative concerns are manageable when addressed early.
Maintaining gauze pressure
Following your extraction, some gauze to bite down on will be placed over the extraction site. By biting down and maintaining pressure on the gauze as instructed, any active bleeding should stop. You may change the gauze pad after the first hour. Continue to bite down for another 45 minutes if heavy oozing continues. While it's normal for a little oozing to continue for 24 hours, contact our office if you are still experiencing profuse oozing or bleeding.
Until the local anesthesia wears off
Until the local anesthetic has completely worn off, it's essential to protect yourself from unintentionally biting or injuring your lips, cheeks, gums, or tongue.
Take medications as prescribed
Antibiotics:
If you have been given a prescription for antibiotics, be sure to take the correct dosage and full course of medication as prescribed.
Pain management:
It's helpful to take a pain reliever before the local anesthetic completely wears off. Over-the-counter (non-aspirin) pain medication may be taken to relieve discomfort. Any prescription pain medication should only be taken as directed.
To facilitate healing
Do not rinse your mouth, spit, drink through a straw, or suck on candies. It's essential to allow the extraction site to clot and not dislodge the new clot once it has formed.
Applying ice
An ice-pack held in place in the facial area overlying the extraction site helps to control swelling. Apply the ice for 10-minute intervals during the first day following your procedure.
Avoid smoking
Smoking not only prevents clot formation, but it also interferes with healing. Avoid smoking and tobacco products for the first week.
Watch what you eat and drink
Stay away from hot or spicy foods and drinks for the first day or two. Also, refrain from drinking any carbonated or alcoholic beverages. Stick with a diet of soft foods and liquids for the first couple of days following surgery. Drink plenty of fluids.
Oral hygiene
Brush gently; it's essential to take great care not to disturb or irritate the extraction site for a few days. A very mild lukewarm saltwater solution can be used to freshen your mouth. Remember not to rinse or spit that first day or two. Simply let any liquids gently fall from your mouth into the sink.
An appointment for a follow-up visit
If sutures (stitches) were placed, or if a complex extraction, an infection, or other issues requires a visit to monitor your healing and progress, you will be given an appointment for follow-up care. It's essential that you keep this appointment as provided.
If you experience continued bleeding, ongoing pain, more swelling, have a bad taste in your mouth, or other unusual symptoms, contact our office.
When a tooth must be removed, you deserve skilled care that addresses both the procedure and your long-term oral health. Our team at Studio Dental Center for Advanced Dentistry focuses on precision, patient comfort, and clear guidance about replacement options so you can make informed decisions about restoring form and function when you’re ready.
After extraction, we will review the most appropriate restorative choices for your situation—whether that involves a removable denture, a fixed bridge, or implant-supported options. If implants are considered, we’ll discuss timing, bone preservation strategies, and the steps involved in that treatment pathway so you understand the full sequence of care.
Our goal is to help you move forward with confidence, armed with realistic expectations and a clear plan. If you have questions or want more information about extractions or tooth replacement solutions, please contact us to speak with a member of our team.

A tooth extraction may be recommended when saving the tooth would jeopardize your oral health or when the tooth is causing pain or recurrent infection. Common reasons include extensive decay that cannot be restored, advanced periodontal disease with loss of support, severe fractures, impacted wisdom teeth, or over-retained primary teeth that block eruption. Extractions are also part of some orthodontic plans when space is needed to align teeth properly. Every recommendation weighs the benefits of retaining the natural tooth against the risk of ongoing disease or damage to neighboring teeth.
Your dentist evaluates the whole picture — clinical findings, imaging, and medical history — before advising removal. When preserving the tooth is feasible, conservative treatments such as root canal therapy or restorative crowns are considered first. If extraction is the most predictable way to stop infection, prevent shifting, or relieve pain, the team will explain the rationale and next steps.
At the office of Studio Dental Center for Advanced Dentistry, the decision is based on a comprehensive clinical exam, a review of your medical history, and appropriate imaging. Digital radiographs and, when indicated, CBCT scans reveal root anatomy, bone levels, and the relationship to nerves or sinuses. We also consider existing restorations, previous endodontic treatment, and the long-term prognosis of the tooth within your overall treatment plan. This information helps the dentist determine whether conservative care or removal is the safer, more predictable option.
When a tooth may be salvageable, options such as root canal therapy, post-and-core buildup, or crown restoration are discussed. In other cases, extraction with planning for replacement is recommended to protect adjacent teeth and oral health. If a case requires a higher level of surgical expertise, we will coordinate a referral to an oral and maxillofacial surgeon while maintaining clear communication throughout care.
A simple extraction applies to teeth that are fully visible in the mouth and have uncomplicated root anatomy; these teeth are typically removed using elevators and forceps after local anesthesia. Because the procedure involves minimal tissue manipulation, recovery is often quicker and less complex than surgical extractions. Simple extractions are commonly used for primary teeth, loose permanent teeth, and single-rooted teeth with straightforward anatomy. Your dentist will confirm the approach after evaluating radiographs and clinical access.
Surgical extractions are necessary when a tooth is broken at the gumline, impacted, fused to the bone, or has complex root morphology that limits access. These procedures often require a small incision in the soft tissue and, in some cases, removal of a small amount of bone to free the tooth. Surgical removal may also involve sutures and a longer, more closely monitored recovery period, and we will explain whether referral to a specialist is recommended.
Local anesthetic is standard for most extractions and effectively prevents pain during the procedure by numbing the immediate area. Topical anesthetic may be applied first to reduce discomfort with the injection, and the dentist verifies complete numbness before starting. For patients with dental anxiety or for more complex surgical cases, additional sedation options are available to help you stay relaxed and comfortable. The choice of sedation is guided by the patient's medical history, the expected complexity of the extraction, and informed consent.
Common supplemental options include nitrous oxide for light sedation, oral sedatives for moderate relaxation, and monitored IV sedation for deeper sedation when appropriate. Some forms of sedation require pre-procedure instructions such as fasting and a responsible adult to drive you home after the appointment. Your dentist will discuss the risks and benefits of each option and recommend the safest approach for your situation.
Before your extraction appointment, provide an up-to-date medical history and a complete list of medications to the dental team so they can identify any factors that may affect healing or bleeding. If you are taking blood thinners or have medical conditions that could impact the procedure, your dentist may request medical clearance or coordinate care with your physician. Follow any preoperative instructions related to fasting if sedation is planned, and arrange for transportation if you will receive moderate to deep sedation. Wearing comfortable, loose clothing and avoiding heavy meals immediately before sedation helps maintain safety and comfort.
Plan to have a responsible adult accompany you home if you receive sedatives that impair coordination or judgment. Bring a list of questions, prior imaging if available, and any necessary paperwork to your appointment to streamline care. Avoid smoking for at least 24 hours before the procedure when possible, as tobacco use can interfere with anesthesia and healing.
On the day of the extraction, the team will review your medical history, confirm consent, and ensure the treatment area is fully anesthetized before beginning. During a simple extraction the dentist uses controlled pressure and instruments to loosen the tooth from its ligaments and remove it with minimal trauma to surrounding tissues. If a surgical approach is needed, you may receive additional local anesthesia and, when planned, sedation to maintain comfort throughout the procedure. Throughout the appointment the team monitors your comfort and provides clear instructions about what to expect at each stage.
After the tooth is removed, the socket may be irrigated, shaped, and, when indicated, closed with sutures to promote healing. Gauze will be placed to control bleeding and you will receive specific post-op instructions tailored to your procedure and sedation status. A follow-up appointment will be scheduled if stitches were placed or if ongoing monitoring is recommended.
Most patients experience the greatest discomfort and swelling during the first two to three days after extraction, after which symptoms typically begin to improve. Maintaining the recommended gauze pressure, using ice during the initial 24 hours, and following medication instructions help control bleeding and reduce swelling. Mild pain and light oozing are common and usually resolve with proper care and rest. If healing proceeds normally you should see steady improvement each day and be able to return to regular activities as comfort allows.
Soft tissue closure and initial healing generally occur within one to two weeks, while the underlying bone remodels over several months. If you are planning tooth replacement such as an implant or bridge, your dentist will discuss timing and any bone preservation measures that may be recommended. Keeping follow-up appointments ensures the site is healing as expected and allows timely planning for restorative care.
To reduce the risk of dry socket and infection, avoid actions that could dislodge the forming blood clot such as rinsing vigorously, spitting, or using a straw for the first 24 to 48 hours. Do not smoke or use tobacco products for at least a week after extraction because nicotine and suction can interfere with clot formation and healing. Maintain gentle oral hygiene, taking care to avoid the extraction site while keeping the rest of your mouth clean to limit bacterial buildup. If antibiotics or antimicrobial rinses are prescribed, take them exactly as directed to reduce infection risk.
Eat soft, cool foods and avoid hot, spicy, or crunchy items that might irritate the socket during the early healing phase. Follow prescribed pain management to keep discomfort controlled and avoid overuse of nonrecommended medications. Contact the office promptly if you experience sudden worsening of pain, a foul taste, or prolonged heavy bleeding so the team can evaluate and treat any complications.
After a tooth extraction there are several restorative pathways to consider, and your dentist will help you choose the option that best preserves function and appearance. Options commonly include a removable partial denture, a fixed dental bridge that uses adjacent teeth for support, or an implant-supported restoration that replaces the tooth root and crown. In some situations immediate temporary solutions can restore appearance while planning proceeds for a definitive restoration. The condition of the surrounding bone and soft tissue influences timing and the most suitable treatment sequence.
If an implant is a potential option, bone preservation strategies such as grafting may be recommended to support future implant placement and long-term stability. Your dentist will discuss the benefits and timing for immediate versus delayed replacement based on healing and overall treatment goals. A coordinated plan ensures restorative needs are integrated with extraction, whether the treatment occurs in the general practice or involves referral to a surgical specialist.
You should contact the dental office promptly if you have persistent heavy bleeding that does not respond to gauze pressure, increasing pain that is not controlled with prescribed medication, or swelling that worsens after the initial two to three days. Other reasons to seek immediate attention include fever, a bad taste or smell from the extraction site that suggests infection, or prolonged numbness in the lip, tongue, or chin. If you receive sedation and experience unexpected complications after leaving the office, contact your caregiver and the clinic so they can advise next steps and coordinate care. For urgent concerns the team can determine whether an in-office evaluation, antibiotics, or a referral is needed to resolve the issue quickly.
When in doubt, call the office to describe your symptoms so the staff can triage your situation and recommend whether you need an urgent appointment. The team at Studio Dental Center for Advanced Dentistry will provide guidance and schedule follow-up as needed to ensure safe recovery and appropriate next steps. Timely communication helps prevent minor problems from becoming more serious and supports predictable healing.

Ready to book your next dental visit or have questions about your care?
At Studio Dental Center for Advanced Dentistry, our team is here to make getting started simple and stress-free. Whether you call, email, or submit our online form, we’re happy to help with scheduling, treatment questions, or anything you need along the way. We take the time to listen and guide you through your options so you feel confident and informed at every step. Take the first step toward a healthier, more confident smile, reach out today and experience personalized care made easy.